The Story of My Mysterious Pain
I never talked about my pain.
For a start, it sometimes hurt too much to talk about anything. On bad days, any movement of my mouth—to speak, to eat, to brush my teeth—could trigger a jolt like an electric shock across the right side of my face. It felt like my cheek and lower jaw had been taken over by the vengeful Norse god Thor, who defended his turf with an endless supply of lightning bolts.
But even on good days, there wasn’t much I could say. Pain isn’t an inspiring topic for conversation. In an odd way, it’s like music—words always fall far short of conveying its essence.
If you want to support my work, please take out a premium subscription (just $6 per month).
I’m reminded of the famous meeting, in May 1922, of the two towering modernist novelists of the era, James Joyce and Marcel Proust, at the Majestic Hotel in Paris. Igor Stravinsky, Sergei Diaghilev, Pablo Picasso, and William Carlos Williams were also in attendance. But at one point, the two literary lions huddled together in conversation.
What did they talk about? Were they planning the future of the novel? Were they exchanging tips for handling writer’s block?
Not in the least. They were both complaining about their medical problems. No words about arts or culture were exchanged. According to William Carlos Williams, the conversation went like this:
Joyce said, “I’ve headaches every day. My eyes are terrible.”
Proust replied, “My poor stomach. What am I going to do? It’s killing me. In fact, I must leave at once.”
“I’m in the same situation,” replied Joyce. “If I can find someone to take me by the arm. Goodbye!”
“Charmé,” said Proust. “Oh, my stomach, my stomach.”
That’s what pain does. It reduces even the most eloquent to moaning and groaning.
Even if I’d limited myself to precise clinical details, there still wasn’t much to say. For the first three years, I didn’t have a name for my affliction or any idea what caused it. I couldn’t even find the right words to describe my symptoms.
“I finally figured out the cause of my pain. But that was just the first step. I had more to take—and three weeks ago they led me to an operating table at Columbia Presbyterian Hospital in Manhattan.”
That’s because my pain kept changing. Thor had turned into a major league pitcher with an endless variety of fastballs, sliders, curveballs and change-up pitches. The pain moved from spot to spot—although it was always somewhere on the lower right side of my face, the metaphorical home plate for this agonizing sport.
How could I even begin to explain this to a doctor? I couldn’t even answer that simplest of questions: Where does it hurt? It never stayed in one place long enough to establish a routine.
The same was true of the type of pain. Some days it burned like a fire. Other days it throbbed like a toothache. It was endlessly creative.

It first struck one day during the COVID lockdown—while I was eating lunch, I felt ten seconds of intense fire in my teeth. I actually let out a shout. That’s how bad it was.
The pain was over in a flash, but it returned sporadically over the next few days. I assumed I had some dental emergency. But at a hastily arranged appointment, the oral surgeon assured me that my teeth were fine—maybe I was just biting too hard.
I’ve heard of others with my condition who didn’t find out what was really wrong until they had two or three teeth pulled. As it turns out, this affliction can’t be fixed by any dental procedure.
Just when I was at my wit’s end, the pain disappeared completely—as mysteriously as it had arrived. And it stayed in hiding for the next fourteen months. But when it came back, it was worse than ever.
In its new guise, the pain woke me up every morning around 6:30 AM. This time it was the worst pain I’ve ever experience in my life—as if my right cheek had been set on fire.
The first time this happened, I jumped out of bed and ran to get an ice pack from the freezer. I pressed the ice pack to my face and—surprise!—this just made the pain even worse. I’m fortunate that the fire only lasted around sixty seconds, but if I tried to go back to sleep, it could happen again a few minutes later.
My nights now became perilous. I found that the only way to sleep without risk was to remain absolutely motionless on my back—even the slightest movement could bring on another attack.
I now knew that I needed to take action. But what kind of action? I still didn’t know what was wrong with me. But I did possess one skill that could help—I’m very good at doing research. So I set myself the task of diagnosing myself.
A few months later, when I laid it all out for my neurologist, she was amazed. “Are you a professional medical researcher?” She asked.
“No,” I replied. “But I am a writer, and I have spent most of my life doing research of various sorts.”
“Well, what you did was impressive.”
Yes, I had finally figured out the cause of my pain. But, as it turned out, that was just the first step. I had several more to take—and three weeks ago they led me to an operating table at Columbia Presbyterian Hospital in Manhattan.
My affliction is called trigeminal neuralgia. Here’s what I learned about it from various sources.
“Trigeminal neuralgia is a rare and extremely painful condition.”
and
“The pain is often described as excruciating, like an electric shock. The attacks can be so severe that you’re unable to do anything while they’re happening.”
and
“When severe, it is the most excruciating pain known to man. This pain most frequently involves the lower lip and lower teeth or the upper lip and cheek, but it also may involve the nose and the area above the eye.”
and
“The emotional strain of living with repeated episodes of pain can lead to psychological problems, such as depression. During periods of extreme pain some people may even consider suicide.”
and
“Trigeminal neuralgia usually affects one side of the face….It can be progressive, with attacks often worsening over time, and fewer and shorter pain-free periods before they recur. Eventually, the pain-free intervals disappear, and medication to control the pain becomes less effective.”
All of this was alarming. But the last point was especially worrisome. There is just one medication approved for treatment, but it loses efficacy over time.
My experience backed up this claim. At first, the pills stopped the pain entirely, but a few months later it started coming back. Even larger doses (which caused alarming side effects) couldn’t put out the fire.
I met with another specialist who warned me: “Don’t fool yourself. This is a progressive disease. It gets worse over time, and you will exhaust what medicine can do for you.”
This motivated me to do still more research. I explored every possible kind of treatment, even the crankiest. Could cyberknife radiation help me? How about injecting botox into the trigeminal nerve? There was some guy in Colorado who touted plasma-enriched platelets. Another eccentric insisted that the capsaicin in hot peppers would do the trick—on the principle that you fight fire with fire.
But my research identified problems with every one of these options. None of them could promise me lasting relief.
I eventually learned that there was one procedure with a high success rate. But it required a highly trained neurosurgeon, who would open up a hole in my skull (behind my right ear)—and then remove points of compression on my trigeminal nerve.
And, of course, there were risks. Some people don’t survive the surgery. But what other realistic options were there for me? Anything was better than living with this pain.
By the way, I did possess one useful bit of knowledge about neurosurgery, and it proved invaluable. My father had a brain tumor removed when he about the same age I am now. And he was determined to find the best surgeon in the world to undertake the procedure.
So that brought him to Stanford Medical Center, where the head of neurosurgery, John ‘Jake’ Hanberry. removed a tumor (which proved benign) and helped my dad mount a full recovery.
I decided back then that, if I were ever in a similar situation, I would do whatever I could to find the best surgeon. Little did I realize that I would actually need to put that vow into practice.
This led me to the person who could give me my life back.
As a young man, Raymond Sekula studied Latin and Greek, and planned on becoming a classics professor. But during his third year of college, his volunteer work brought him face-to-face with a man who had found relief from Parkinson’s disease after an experimental surgery.
“And after that,” he explains, “I just decided: this is what I wanted to do with my life. And so that’s how I really got interested in medicine.” But one part of Sekula’s initial plan came true—he did become a professor. He is now Professor of Neurological Surgery at the Neurological Institute at Columbia University.
My surgeon literally wrote the textbook on the surgery I needed—it’s called microvascular decompression. He has performed this procedure more than two thousand times, and is responsible for many innovations along the way.
He’s also a caring, compassionate man. His entire staff is that way too. They got me on his schedule, even though I was thousands of miles away, and helped me at every step.
At our initial conversation, Dr. Sekula told me that my MRI looked promising. He had identified an artery that was the likely source of compression on my trigeminal nerve. If he could remove that pressure, I had an excellent chance for lasting pain relief.
So Tara and I flew into New York on March 1 and moved into a hotel near the hospital. At noon on March 4, I went into surgery, and Dr. Sekula worked his magic.
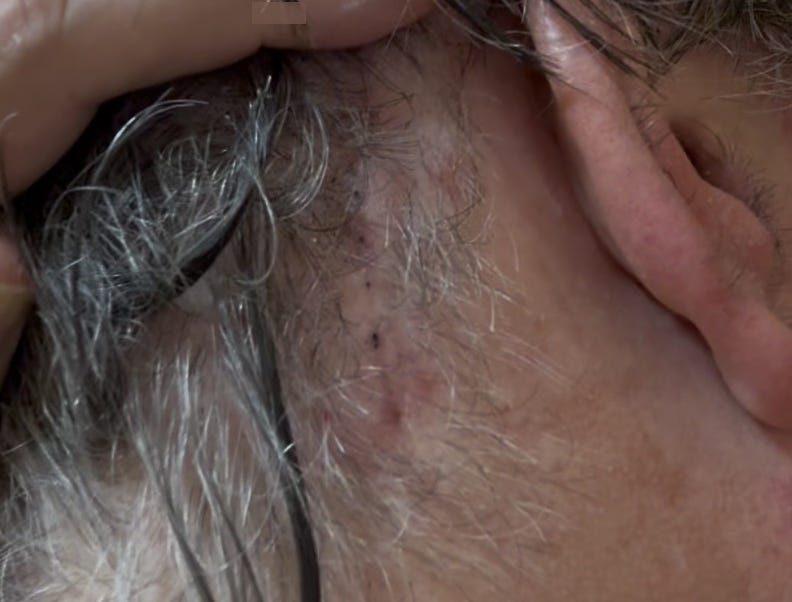
He did it with an impressive degree of elegance. He was able to do everything through an opening the size of a nickel. He identified and removed two points of compression. The incision would hardly be noticed by an outside observer—and he even did it in such a way that I could comb my hair over it, hiding it completely from view.
This is what it looked like yesterday (three weeks post-surgery).
But the best news is this—my pain is gone.
I noticed that immediately after regaining consciousness. There was total radio silence from the trigeminal nerve—and it hasn’t given a tingle or a throb since then. A week after the procedure, I stopped taking the medication I’d been using, and waited uneasily to see if the pain would return. But it didn’t.
Thor is subdued. His lightning bolts no longer disturb my days and nights.
Of course, there’s no guarantee that the pain won’t return, but Dr. Sekula tells me that the odds are in my favor—“even after forty years, the success rate shouldn’t fall below 80 percent”—and he will continue to track my progress in the months ahead.
But now I have my life back—for the first time in years. It feels like a miracle.
In my last conversation with my doctor, I told him that he had given me a gift I could never repay. “If I can ever do anything in return,” I promised, “just let me know.”
He said there was one thing I might consider. Other people suffer from this condition, and many of them deal with the same uncertainty I faced—struggling to identify the cause and learn about treatment options.
Dr. Sekula remembered that I had mentioned, at our first meeting, that I was a writer. Maybe I could do some good, he said, by writing about my experiences. Others might benefit from it.
And that is why you’re reading this story about my mysterious pain. It’s no mystery anymore. Nor is it even a pain, just a memory now. But for some, it still is a reality—and a terrible one.
I hope others can take some comfort in my story, or maybe even find guidance and relief. There are still some happy endings in our health struggles. By sharing mine, maybe I can help others find one too.
For more information on trigeminal neuralgia and related disorders, please visit the website of the Facial Pain Association.




The miracles of our lives are scientists, philosophers, teachers, artists physicians, and others who work everyday to make the world better for others. Oh, to be one like your doctor.
This was deeply familiar to me. One of the hardest things about chronic pain is that you don’t “get used to it” in any noble or uplifting sense, you just become skilled at organising your life around it. That’s a different thing entirely. And when it vanishes, even for a few minutes, the feeling is extraordinary, because you suddenly remember that the world is not supposed to hurt all the time. Those moments feel less like comfort than revelation. Thank you for writing this. People talk a lot about pain as a symptom, but not enough about how it colonises time, attention, sleep, language, and hope. Gioia describes exactly that kind of overwhelming, hard-to-explain pain, and the relief he felt after successful surgery.